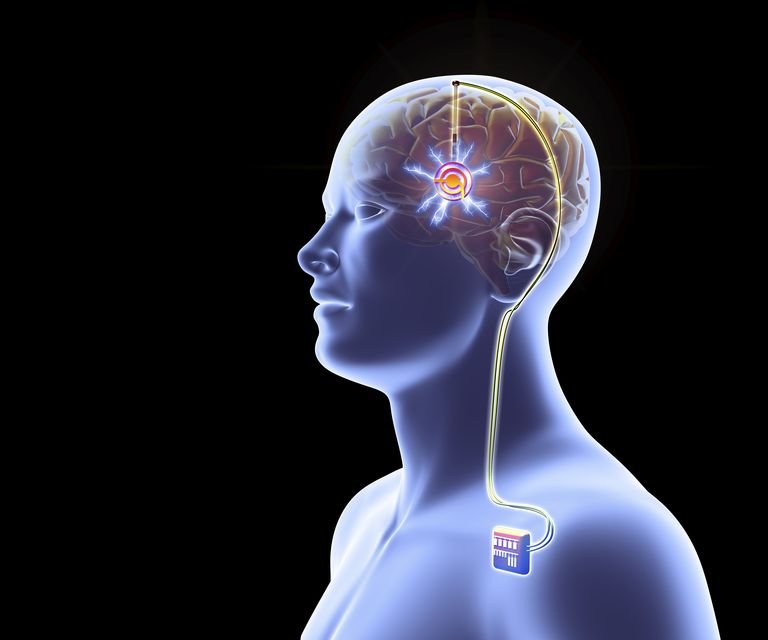
Deep brain stimulation (DBS) therapy can provide long-term symptom improvement for Parkinson’s disease sufferers, according to recent research.
Parkinson’s Patients Might Benefit From Deep Brain Stimulation Therapy
Researchers discovered that individuals who underwent DBS, which requires surgical implantation, experienced considerable improvement in motor symptoms and used less medication over 15 years.

According to senior researcher Dr. Moro, head of the Movement Disorders Unit at Grenoble Alpes University, France, the study demonstrates the efficacy of deep brain stimulation in the very long term for the first time, 15 years after surgery and 25 years following Parkinson’s diagnosis.
According to her, people may notice improvement after an average of 15 years following surgery as compared to before surgery. Furthermore, they could still see a significant reduction in anti-medication Parkinson’s and an increase in quality of life compared to before the intervention.
Parkinson’s disease patients no longer produce dopamine, which impairs their speech, movement, and balance. However, the medicine levodopa, which temporarily replenishes dopamine, can help to alleviate symptoms.
However, because dopamine levels fluctuate throughout the day, patients may have dyskinesia, a levodopa side effect that causes twisting, swaying, or head bobbing.
Deep brain stimulation controls Parkinson’s symptoms by implanting electrodes in specific parts of the brain. The electrodes are connected to a pacemaker-like device inserted under the skin in the upper chest that sends an electrical pulse to help regulate symptoms. Many patients utilize a portable controller to alter the degree of stimulation as needed.
Moro’s team gathered information on 51 DBS participants for the research. They kept the gadget for an average of 17 years.
When data from before the implant was compared to data from 15 years afterwards, the number of times patients had dyskinesia was reduced by 75%. The use of drugs to manage dopamine levels was decreased by 51%, and the period when medication was no longer effective was decreased by 59%.
Researchers discovered just a few minor negative effects after using the gadget for 15 years, and they were mainly treatable.
DBS is indicated for severe Parkinson’s disease, and Moro believes surgery should not be postponed if motor function and quality of life deteriorate despite previous treatments.
This knowledge is important for clinicians, patients, and their families when deciding on a surgical option to treat Parkinson’s disease, she says. In addition, people with Parkinson’s disease should be aware that the benefits of deep brain stimulation surgery will persist for more than 15 years.
As per Dr. Michael Okun, national medical consultant for the Parkinson’s Foundation, DBS has long-term effects in certain individuals when combined with drugs. He was not a participant in the research.
According to Okun, chairman and professor of neurology at the University of Florida, these long-term investigations reveal many things. The most crucial message they convey is that illness progresses despite intervention.
Deep brain stimulation and medicine are not cures for the illness. Long-term benefits include dyskinesias and motor irregularities, according to Okun.
Patients who respond well to levodopa, he says, are more likely to benefit from DBS.
Patients who are still benefiting from the device after 15 years are those who have a gradual progression of their sickness. People whose Parkinson’s disease advances faster aren’t around to be tested after 15 years, according to Okun.
He stated that they have patients in their offices who have had Parkinson’s disease for 30 years or more. The essential lesson of deep brain stimulation is to pick people who respond well to levodopa before implanting them.
Okun claims that DBS is bad for walking, talking, thinking, and balancing.
He claims that it helps in the long run by smoothing out variations and decreasing tremors and trembling. It’s encouraging for characteristics that still respond to dopamine, so if their rigidity or stiffness responds to dopamine, it’ll be beneficial. That’s where it’ll make the most noise in 15 years.
Okun emphasized once more that Parkinson’s disease advances regardless of treatment.
What they discovered in the deep brain stimulation populations is that they are still prone to dementia, so they are just like ordinary Parkinson’s disease patients, with walking, talking, and thinking issues that are not successfully addressed by this hardware approach, according to Okun.