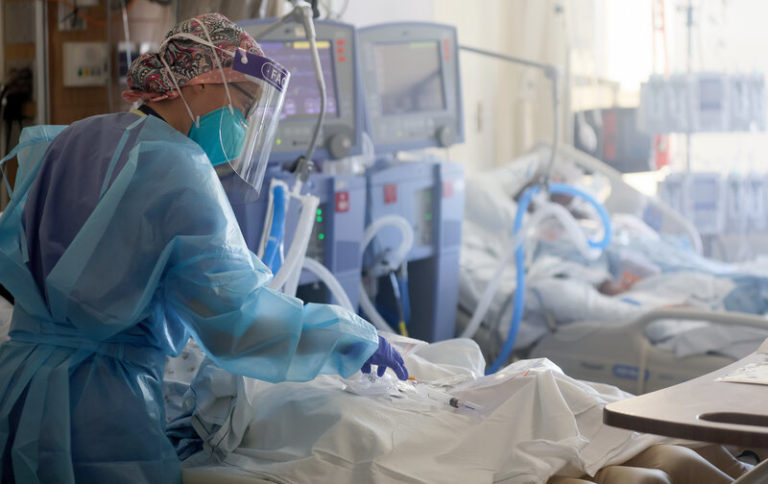
In 2020, insurance companies generously waived cost-sharing to dampen the effects of Covid. In 2021, this is not the case. Most insurance companies are likely to drop these waivers, and as a consequence of this, subscribers will be required to pay humongous chunks of Covid testing and treatment costs.
How Cost-Sharing Waivers Can Reduce The Financial Burden On Americans
Therefore, being hospitalized in 2021 will turn out to be more expensive for the patient and not the insurance company.
According to a study by Kaiser Family Foundation, half of the people who have enrolled on insurance schemes will have their cost-sharing waived off by the end of the year.
After trials have shown that the three vaccines available in the country effectively prevent Covid from turning into diseases that will get you hospitalized, the Food and Drug Administration has given emergency authorization.
A registered nurse, Mary Ann Hart, said that these cost-sharing waivers had protected public health by encouraging people to find out if they have contracted the virus by taking a Covid test either at home or at a hospital.
Easing of Restrictions
As restrictions are continuously eased for people that have been vaccinated, a majority of people who have been admitted to hospitals are yet to be vaccinated.
MedRxiv recently published a research that looked at 4000 patients that had been hospitalized with Covid and found that nearly 71% of patients that had been privately insured and nearly half of Medicare Advantage patients spent $788 and $277 on average, respectively in out-of-pocket costs for facilities and services.
This implies that some saw bills that were even higher than the figures above.
A University of Michigan research team found that out-of-pocket spending exceeded $4000 for around 2.5% of privately insured patients, while 0.2% of Medicare Advantage patients spent more than $4000.
Their findings advocated that cost-sharing waivers may not reach all patients hospitalized, and their out-of-pocket costs could mount even higher should insurers stop the waivers.
The Michigan team opined that federal policymakers should consider making it mandatory for insurers to waive cost-sharing for whatever hospitalization is related to Covid throughout the pandemic rather than voluntarily relying on insurers to do away with this financial weight.
In March 2020, former President Donald Trump signed the CARES Act, and this law required all insurers to cover Covid testing and vaccinations and all Covid treatment costs for patients of Medicare.
When the pandemic struck, procedures involving elections and surgeries and other care that were not urgent were delayed, eliminating the usual claims for insurance and making the companies extra profitable. This gives more reason to make insurance companies bear the costs.
America’s Health Insurance Plans has put together an exhaustive list of what insurers are offering waivers. This list is available on their website.
The Actual Cost of Hospitalization
Economists at Harvard have estimated that by November, Covid would have cost the country approximately $16 trillion. This number includes vaccination, deaths due to unwillingness to seek medical aid, Covid deaths, and mental health impact.
If an average American was hospitalized for over 15 days, he would owe a $5000 deductible and a 20% coinsurance.
Clearly, the removal of these cost-sharing waivers will be largely burdensome to the patient and their family. An average American cannot afford to get sick with Covid.
James Papesca, a faculty of nursing, said that he does not believe that there is any sort of advantage for insurance companies to voluntarily extend the cost-sharing waivers as people who have been vaccinated against Covid are returning to situations that existed before the pandemic, which includes a usual activity.